March 12, 2026 Legislative Update
Legislative Update
March 12, 2026
Jan Lanier, JD, RN
Introduction
Members of the General Assembly have been busy attending committee meetings as chairs have scheduled numerous bills for hearing to clear their desks of a backlog of pending legislation. Pursuant to rules adopted by both chambers at the beginning of each new session, all bills introduced by a specific date (usually sometime in March or April) MUST receive at least one committee hearing. For minority party members, it is a way to ensure their proposals receive at least cursory attention. It can signal the issues these members believe are important to put forward even though they are unlikely to advance past hearing number one. The majority party is also eager to see its issues discussed by a committee, but the strategy serves a slightly different purpose. Both parties are looking toward the fall election and trying to set priorities that will appeal to their voters. This is especially true for proposals that are more cultural and philosophical in nature. Since mid- December forty new bills have been introduced in the senate and 97 in the house. Between both chambers over 1000 bills have been introduced so far and there will be more!
Bills of interest
A recent addition in the house is HB 718 jointly sponsored by Reps. Karen Brownlee (D-Cincinnati) and Jodi Salvo (R-Zoar). It addresses “qualified mental health specialists” (QMHs) who work in behavioral health but are currently unlicensed. QMHs serve as case managers or peer coordinators. According to bill sponsor Rep. Brownlee, “They are often key to bringing together all the resources and environmental needs that help a kid or family to have good mental health outcomes.” (Source: Kano, K. (2/27/26) Legislation aims to certify care coordinators. State Affairs, Gongwer-Ohio). The bill would impact Medicaid reimbursement for the covered services that currently is dependent on where the QMH is employed. Eligibility for reimbursement must be newly determined with each job change, a process that can take months according to Brownlee. The bill also creates a pathway for providers to have a formalized training process that has three levels that could encourage people to make care coordination a long-term career. Currently, there is no state oversight of these individuals. With passage of the bill, however, that oversight would be undertaken by the Chemical Dependency Professionals Board whose name would be changed to the Behavioral Health Professionals Board. (Ibid.)
Another bill that is receiving attention is one that addresses a subject that has been before legislators numerous times in previous general assemblies. HB 537 jointly sponsored by Reps. Riordan McClain (R-Upper Sandusky) and Melanie Miller (R-Ashland) would regulate and license midwives and make changes to freestanding birthing centers. The House & Human Services Committee agreed to accept a substitute bill rather than work from the as introduced version. Therefore, sponsor testimony focused on the new version; and the starting point for future work should take into consideration the changes interested parties have already agreed to make to the original bill.
In addition to certified nurse midwives who are regulated by the Board of Nursing, the bill defines “certified midwives, licensed midwives, and traditional midwives” that according to joint sponsor Rep. Riordan already exist without official state recognition or regulation. Under the bill, licensed and traditional midwives would be under the auspices of the Department of Commerce, a factor that some nurses have questioned because of the subtle message it sends, and the potential for conflicting regulatory standards and public confusion.
The regulatory scheme the bill creates is confusing so the PPC has reached out to nurse midwives, women’s health care providers, and nurse educators to get their perspectives.
HB 535 sponsored by Rep. Brian Lorenz (R-Powell) addresses nurse staffing issues by building on current law that established nurse-led staffing committees made up largely of direct care nurses. The bill does not include specific nurse to patient staffing ratios, leaving it to individual hospitals to determine the numbers based on nationally accepted evidence-based standards that factor in many key variables (identified in the bill) that determine staffing needs. The bill does include penalty language for facilities that do not comply; however, the penalties may be more lenient than some groups would prefer and stricter than others would like. Sponsor testimony took place in the health committee on January 11th.
Rep. Lorenz described the bill as building on existing law and a step forward that includes balanced accountability for the parties. He alluded to his family’s experiences having a wife who is a nurse and also a mother of their three children. She often arrived home after work exhausted and concerned that she hadn’t done enough for her patients. Rep. Lorenz said he had worked with ONA and OHA on the bill and their input regarding best practices have been reflected in the bill. None of the committee members had questions for him.
Another staffing bill (HB 521) sponsored by democrats Reps. Crystal Lett (Hilliard), and Christine Cockley (Columbus) has not yet been scheduled for a hearing. It was referred to the health committee on 10/22/25 and does include specific nurse to patient ratios.
HB 508, phases out the currently required standard care agreement that has limited APRN practice for years. The bill is before the ouse Medicaid committee chaired by Rep. Jennifer Gross, (R-West Chester) one of the bill’s sponsors along with Rep. Rachel Baker (D-Cincinnati). Rep. Gross believes she has the votes in committee to get the bill favorably recommended for a vote by the full house. She asked that ANA-Ohio encourage its members to communicate with their legislators to urge passage of the bill. (Source: Kano, K. (3/11/26) Gross confident her version of APRN independent practice bill will win out. State Affairs, Gongwer-Ohio.)
HB 449, sponsored by republican Reps. Tim Barhorst (Fort Loramie) and Riordan McClain (Upper Sandusky,) also phases out the Standard Care Agreement (SCA) but requires only 2,000 hours of practice before the APRN is no longer required to have an SCA in place. The bill had sponsor testimony before the health committee on March 11th. Sponsors emphasized the money some APRNs are forced to pay to a collaborating physician to enter into an SCA. Sponsors noted that these contracts can cost as much as $100,000 per year. While the state mandated requirement was well-intentioned initially, it is no longer needed and prevents APRNs from meeting health care needs in areas with significant health care shortages. Committee members had questions about what is required by law to be included in the SCA, and Rep. McClain emphasized that the bill is permissive meaning health systems could still require the SCA if they wanted to. Rep. Anita Somani (D-Dublin) a physician who has opposed the bill, and others like it in past general assemblies, asked for data about whether better access to APRN care reduces costs or do the APRNs order more tests and labs than physicians need to order thereby driving up costs. She also asked whether APRN over-prescribing is another cost driver. Committee chair Rep. Jean Schmidt (R-Loveland) asked about the alleged shortage of physicians willing to enter into SCAs. She said there are over 20,000 potential collaborators and each physician may collaborate with five APRNs, so the shortage seems exaggerated. She also sought data regarding the increased access to care that occurs in states where there is no SCA requirement in place.
HB 52 dealing with CRNA practice was passed unanimously in the senate and signed by Governor DeWine on March 10, 2026. It will become effective in 90 days. According to the bill’s sponsor, Rep. Kellie Deeter (R-Norwalk) who is a CRNA, “It took 12 years to get this bill passed.” It serves as a good example of what can be accomplished when nurses are elected to the general assembly.
SB 230, the so called “test to treat” bill allows pharmacists to order lab tests and prescribe medication for such illnesses as the flu, COVID-19,strep throat and other minor respiratory diseases. The bill’s sponsor Sen. Mark Romanchuk (R-Ontario) believes the bill would relieve congestion in emergency departments and increase access to care in rural and other underserved areas. According to Sen. Romanchuk, test to treat has been enacted and implemented in 20 states with no issues.
Authorizing pharmacists in Ohio to take on these added responsibilities was part of Ohio’s grant application to receive federal funds under the Rural Health Transformation Program (RHTP). The state was awarded $202 million dollars in late 2025, and it remains unclear if the federal government will claw back a portion of those funds if the state fails to make test to treat a reality as promised in the application. The bill is opposed by the Ohio State Medical Association (OSMA). Its spokesperson argued that adding to a pharmacist’s workload will exacerbate access problems. “Turning their attention to this level of patient care will take them away from their primary area of responsibility, filling prescriptions.” (Source: Kano, K. (3/4/26) Health chair predicts passage of test-to-treat bill despite opposition. State Affairs, Gongwer-Ohio). Pharmacists generally support the bill. Senate health chair, Sen. Matt Huffman (Tipp City) believes the bill will become law. In previous hearings, the sponsor assured the three physician members of the health committee that he would work with them to address their concerns about the need to address age limitations, integration of health records, and additional training for pharmacists.
HB 485 sponsored by Rep. Melanie Miller (R-Ashland) requires students in grades 5-12 to view a high-definition ultrasound video and the animated “Meet Baby Olivia” video as part of classes tied to the health curriculum. It received a senate hearing on March 10th. A similar bill (SB 310) is also pending before the senate education committee. The committee chair Sen. Andrew Brenner (Delaware) expressed a preference for the senate version because it is more flexible. The sponsor said she was willing to work with the committee on its concerns as she did in the house. (Source: Gallick, T. (3/10/26) Fetal development education plan likely to see changes in senate. State Affairs Gongwer-Ohio.)
Getting a Handle on Drug Costs:
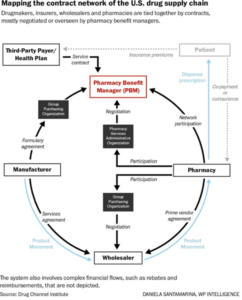
The issue of Pharmacy Benefit Managers (PBMs) is the subject of several proposals before the general assembly including HB 229 sponsored by Rep. Kellie Deeter (R-Norwalk). It has passed both the house and senate and currently awaits Gov. Mike DeWine’s signature. The bill establishes a stand-alone licensing process for PBMs beginning July 1, 2027. Licensure is required if someone solicits a plan sponsor or provides PBM management services. Failure to comply is a 4th degree misdemeanor. The PBM must enter into a written agreement with a plan sponsor before providing PBM management services to the sponsor. Violations of the law could result in a $15,000 civil penalty per violation. PBMs must at least annually account to the plan sponsor any price discounts, rebates, inflationary payments, credits, claw backs, fees, grants, charge backs, reimbursements or any other benefits received by the PBM. The top three PBMs are CVS Caremark (owned by CVS Health which also owns Aetna), Express Scripts (Owned by Cigna), and Optum Rx (owned by UnitedHealth Group). Together they manage 80% of drug claims. (Source: Martin, K. (3/17/25) What pharmacy benefit managers do and how they contribute to drug spending. The Commonwealth Fund. New York, NY.)
Ohio legislators have three bills dealing with PBMs in the current session of the general assembly; HB 229 (see above) SB 210, and HB 192. Like HB 229, SB 210 proposes licensure of PBMs. Sponsored by Sen. Louis Blessing (R-Cincinnati) the bill has received no action from the senate health committee. HB 192 sponsored by Rep. Tim Barhorst (R-Fort Loramie) and Tex Fisher (R-Boardman) addresses the impacts PBMs are having on community and independent pharmacies. The bill was introduced in March 2025 and referred to the house insurance committee. It has had periodic committee hearings, with the next one scheduled for March 11, 2026. Proponents of the bill say PBMs are driving smaller community and independent pharmacies out of business thus creating pharmacy deserts across the state. Retaliation, accreditation, and auditing requests are the tactics being used by PBMs that the bill attempts to address. Retaliation— Low reimbursement rates, making it difficult for lower volume pharmacies to survive. Accreditation--Requiring pharmacies to meet standards that exceed those required by the state board of pharmacy prevents the pharmacy from being part of the PBM network. Therefore, the availability of certain medications is limited, and pharmacy costs increase. Finally, unpredictable frequent audits that include extensive documentation requests without cause or clear explanation, increases the cost of doing business for these pharmacies. The bill bans retaliation and limits accreditation standards to those that are consistent with the board of pharmacy. It also limits the frequency of audits and requires a clear explanation of potential issues.

